Open Resources for Nursing (Open RN)
Catheter Size and Type Selection
Peripheral IV catheters are available in a variety of sizes, most commonly ranging from 14 gauge to 26 gauge. Note that the lower the gauge size, the wider the diameter of the catheter, with 14-gauge catheters allowing for the greatest flow rate.[1] Catheter sizes are color coded to allow for easy identification of the catheter size after a vein is accessed. See Figure 23.12[2] for colors associated with IV catheter sizes and their associated flow rates.

Nurses must consider the purpose for venous access, along with assessment of the patient’s vessel size, when selecting an IV catheter to attempt cannulation. The smallest IV catheter should be selected that will accommodate the prescribed therapy and patient need.[3]
Catheters with a smaller gauge (i.e., larger diameter) permit infusion of viscous fluids, such as blood products, at a faster rate with decreased opportunity for catheter occlusion.[4] Additionally, an appropriately sized catheter also allows for adequate blood flow around the catheter itself. The most common IV catheter size for adult patients is 18- or 20-gauge catheters. However, frail elderly patients and children have smaller vasculature, so a 22-gauge catheter is often preferred.
There are different manufacturer brands of IV catheters, but all include a beveled hollow needle, a flashback chamber in which blood can be visualized when entering the vein, and a flexible catheter that is left in the vein after the catheter has been threaded into the vein and the needle removed.
IV insertion equipment varies among institutions, but common types include shielded IV catheters or winged (i.e., “butterfly”) devices. Variation is often related to the presence of a stabilizing device at the site of insertion, as well as the presence of short extension tubing. For shielded catheter types, the stabilizing device and extension tubing are typically added to the catheter itself and not included with the cannulation needle. See Figure 23.13[5] for an image of shielded IV catheters.
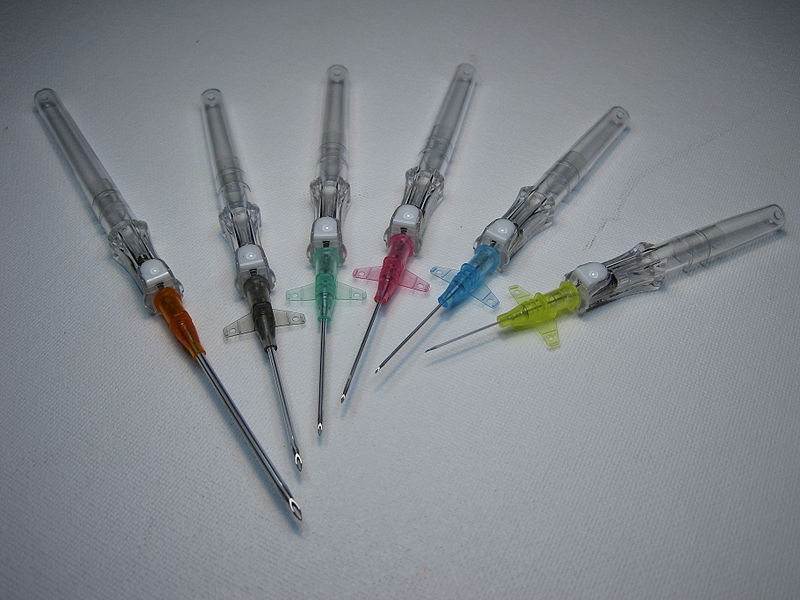
Nurses must ensure the selected size and type of IV catheter are appropriate for the procedure or infusion that is ordered because not all peripheral IV catheters are suitable for all procedures. For example, if a procedure requires the infusion of contrast dye, a specific size infusion port is required.
Despite the wide variation in catheter equipment that is available, there has been significant focus among manufacturers regarding the need for safety equipment during venipuncture. Many devices utilize mechanisms to self-contain needles within a plastic sheath after withdrawal from the patient. These devices can be activated through a button in the devices or a manual trigger initiated by the individual attempting cannulation. Regardless of the type of safety lock, it is important to utilize the equipment as intended and never attempt to disable or override the mechanism. These mechanisms are important to help prevent accidental needlesticks or injury with a contaminated needle after it has been removed from the patient. Additionally, after cannulation is attempted, the individual who attempted cannulation is responsible for ensuring all needles are disposed of in a sharps container. It is good practice to be aware of how many sharps were brought into the room, opened, and disposed. This helps to ensure that any needles are not inadvertently left in a patient’s bed, tray table, floor, etc. Nurses must be familiar with the equipment used at the health care facility and receive orientation on the specific mechanics related to the equipment and safety practices.
Initiating Peripheral IV Access
The steps for initiating peripheral IV access are described in the Open RN Nursing Advanced Skills “Perform IV Insertion and IV Removal” checklist in Chapter 1.
Monitoring for Potential Complications
Several potential complications may arise from peripheral intravenous therapy. It is the responsibility of the nurse to prevent, assess, and manage signs and symptoms of complications. Complications can be categorized as local or systemic. See Table 23.4a for potential local complications of peripheral IV therapy.
Table 23.4a Local Complications of Peripheral IV Therapy[6],[7]
| Complications | Potential Causes and Prevention | Treatment |
|---|---|---|
| Phlebitis: The inflammation of the vein’s inner lining, the tunica intima. Clinical indications are localized redness, pain, heat, purulent drainage, and swelling that can track up the vein leading to a palpable venous cord. | Mechanical causes: Inflammation of the vein’s inner lining can be caused by the cannula rubbing and irritating the vein. To prevent mechanical inflammation, choose the smallest outer diameter of a catheter for therapy, secure the catheter with securement technology, avoid areas of flexion, and stabilize the joint as needed.[8]
Chemical causes: Inflammation of the vein’s inner lining can be caused by medications or fluids with high alkaline, acidic, or hypertonic qualities. To avoid chemical phlebitis, follow the parenteral drug therapy guidelines in a drug reference resource for administering IV medications, including the appropriate amount of solution and rate of infusion. Infectious causes: May be related to emergent VAD insertions, poor aseptic technique, or contaminated dressings. |
Chemical phlebitis: Evaluate infusion therapy and the need for different vascular access, different medication, slower rate of infusion, or more dilute infusate. If indicated, remove the Vascular Access Device (VAD).[9]
Transient mechanical phlebitis: May be treatable by stabilizing the catheter, applying heat, elevating limb, and providing analgesics as needed. Consider requesting other pharmacologic interventions such as anti-inflammatory agents if needed. Monitor site for 24 hours post-insertion, and if signs and symptoms persist, remove the catheter.[10] Infectious phlebitis: If purulent drainage is present or infection is suspected, remove the catheter and obtain a culture of the purulent drainage and catheter tip. Monitor for signs of systemic infection.[11] |
| Infiltration: A condition that occurs when a nonvesicant solution is inadvertently administered into surrounding tissue. Signs and symptoms include pain, swelling, redness, the skin surrounding the insertion site is cool to touch, there is a change in the quality or flow of IV, the skin is tight around the IV site, IV fluid is leaking from IV site, or there are frequent alarms on the IV pump. | Infiltration is one of the most common complications in infusion therapy involving an IV catheter.[12] For this reason, the patency of an IV site must always be checked before administering IV push medications.
Infiltration can be caused by piercing the vein, excessive patient movement, a dislodged or incorrectly placed IV catheter, or too rapid infusion of fluids or medications into a fragile vein. Always secure a peripheral IV catheter with tape or a stabilization device to avoid accidental dislodgement. Avoid sites that are areas of flexion. |
Stop the infusion and remove the cannula. Follow agency policy related to infiltration. |
| Extravasation: A condition that occurs when vesicant (an irritating solution or medication) is administered and inadvertently leaks into surrounding tissue and causes damage. It is characterized by the same signs and symptoms as infiltration but also includes burning, stinging, redness, blistering, or necrosis of the tissue. | Extravasation has the same potential causes of infiltration but with worse consequences because of the effects of vesicants. Extravasation can result in severe tissue injury and death (necrosis). For this reason, known vesicant medications should be administered via central lines. | Stop the infusion. Detach all administration sets and aspirate from the catheter hub prior to removing the catheter to remove vesicant medication from the catheter lumen and as much as possible from the subcutaneous tissue.[13]
Follow agency policy regarding extravasation of specific medications. For example, toxic medications have a specific treatment plan. |
| Hemorrhage: Bleeding from the IV access site. | Bleeding occurs when the IV catheter becomes dislodged. | If dislodgement occurs, apply pressure with gauze to the site until the bleeding stops and then apply a sterile transparent dressing. |
| Local infection: Infection at the site is indicated by purulent drainage, typically two to three days after an IV site is started. | Local infection is often caused by nonadherence to aseptic technique during IV initiation or IV maintenance or the dressing becomes contaminated or non-intact over the access site. | Remove the cannula and clean the site using sterile technique. If infection is suspected, remove the catheter and obtain a culture of the purulent drainage and catheter tip. Monitor for signs of systemic infection. |
| Nerve injury[14] | Paresthesia-type pain occurring during venipuncture or during an indwelling IV catheter can indicate nerve injury. | Immediately remove the cannula, notify the provider, and document findings in the chart. |
In addition to local complications that can occur at the site of IV insertion, there are many systemic complications that nurses must monitor for when initiating peripheral IV access, as well as monitoring a patient receiving IV therapy. See Table 23.4b for a list of systemic complications, signs, symptoms, and treatment.
Table 23.4b Systemic Complications of Peripheral IV Therapy[15]
| Complication | Signs, Symptoms, and Treatment |
|---|---|
| Pulmonary Edema | Pulmonary edema, also known as fluid overload or circulatory overload, is a condition caused by excess fluid accumulation in the lungs due to excessive fluid in the circulatory system. It is characterized by decreased oxygen saturation; increased respiratory rate; fine or coarse crackles in the lung bases; restlessness; breathlessness; dyspnea; and coughing up pink, frothy sputum. Pulmonary edema requires prompt medical attention and treatment. If pulmonary edema is suspected, raise the head of the bed, apply oxygen, take vital signs, complete a cardiovascular assessment, and immediately notify the provider. |
| Air Embolism | An air embolism refers to the presence of air in the cardiovascular system. It occurs when air is introduced into the venous system and travels to the right ventricle and/or pulmonary circulation. Air embolisms can occur during catheter insertion, changing IV bags, adding secondary medication administration, and catheter removal. Inadvertent administration of 10 mL of air can have serious and fatal consequences. However, small air bubbles are tolerated by most patients. Signs and symptoms of an air embolism include sudden shortness of breath, continued coughing, breathlessness, shoulder or neck pain, agitation, feeling of impending doom, light-headedness, hypotension, wheezing, increased heart rate, altered mental status, and jugular venous distension.
If an air embolism is suspected, occlude the source of air entry. Place the patient in a Trendelenburg position on their left side (if not contraindicated), apply oxygen at 100%, obtain vital signs, and immediately notify the provider. To prevent air embolisms, perform the following steps when administering IV therapy: ensure the drip chamber is one-third to one-half filled, remove all air from the IV tubing by priming it prior to attaching it to the patient, use precautions when changing IV bags or adding secondary medication bags, ensure all IV connections are tight, and ensure clamps are used when the IV system is not in use. |
| Catheter Embolism | A catheter embolism occurs when a small part of the cannula breaks off and flows into the vascular system. When removing a peripheral IV cannula, inspect the catheter tip to ensure the end is intact. Notify the provider immediately if the catheter tip is not intact when it is removed. |
| Catheter-Related Bloodstream Infection (CR-BSI) | Catheter-related bloodstream infection (CR-BSI) is caused by microorganisms introduced into the bloodstream through the puncture site, the hub, or contaminated IV tubing or IV solution, leading to bacteremia or sepsis. A CR-BSI is a hospital-acquired preventable infection and considered an adverse event. A CR-BSI is diagnosed when infection occurs with one positive blood culture in a patient with a vascular device (or a patient who had a vascular device within 48 hours before the infection) with no apparent source for the infection other than the vascular access device. Treatment for CR-BSI is IV antibiotic therapy.
To prevent CR-BSI, it is vital to perform hand hygiene prior to care and maintenance of an IV system and to use strict aseptic technique for care and maintenance of all IV therapy procedures. |
- This work is a derivative of StatPearls by Beecham & Tackling and is licensed under CC BY 4.0 ↵
- “Color-coding_of_IV_cannulas.jpg” by Dr.Vijaya Chandar is licensed under CC BY-SA 4.0 ↵
- Gorski, L. A., Hadaway, L., Hagle, M. E., Broadhurst, D., Clare, S., Kleidon, T., Meyer, B. M., Nickel, B., Rowley, S., Sharp, E., & Alexander, M. A. (2021). Infusion therapy standards of practice. Journal of Infusion Nursing, 44(Suppl 1S), S1–S224. https://doi: 10.1097/NAN.0000000000000396.org ↵
- This work is a derivative of StatPearls by Beecham & Tackling and is licensed under CC BY 4.0 ↵
- “IV_Catheters_(9).JPG” by Intropin is licensed under CC BY-SA 3.0 ↵
- This work is a derivative of Clinical Procedures for Safer Patient Care by British Columbia Institute of Technology and is licensed under CC BY 4.0 ↵
- Simin, D., Milutinović, D., Turkulov, V., & Brkić, S. (2018). Incidence, severity and risk factors of peripheral intravenous cannula‐induced complications: An observational prospective study. Journal of Clinical Nursing, 28(9-10), 1585-1599. https://doi.org/10.1111/jocn.14760 ↵
- Gorski, L. A., Hadaway, L., Hagle, M. E., Broadhurst, D., Clare, S., Kleidon, T., Meyer, B. M., Nickel, B., Rowley, S., Sharp, E., & Alexander, M. A. (2021). Infusion therapy standards of practice. Journal of Infusion Nursing, 44(Suppl 1S), S1–S224. https://doi: 10.1097/NAN.0000000000000396.org ↵
- Gorski, L. A., Hadaway, L., Hagle, M. E., Broadhurst, D., Clare, S., Kleidon, T., Meyer, B. M., Nickel, B., Rowley, S., Sharp, E., & Alexander, M. A. (2021). Infusion therapy standards of practice. Journal of Infusion Nursing, 44(Suppl 1S), S1–S224. https://doi: 10.1097/NAN.0000000000000396.org ↵
- Gorski, L. A., Hadaway, L., Hagle, M. E., Broadhurst, D., Clare, S., Kleidon, T., Meyer, B. M., Nickel, B., Rowley, S., Sharp, E., & Alexander, M. A. (2021). Infusion therapy standards of practice. Journal of Infusion Nursing, 44(Suppl 1S), S1–S224. https://doi: 10.1097/NAN.0000000000000396.org ↵
- Gorski, L. A., Hadaway, L., Hagle, M. E., Broadhurst, D., Clare, S., Kleidon, T., Meyer, B. M., Nickel, B., Rowley, S., Sharp, E., & Alexander, M. A. (2021). Infusion therapy standards of practice. Journal of Infusion Nursing, 44(Suppl 1S), S1–S224. https://doi: 10.1097/NAN.0000000000000396.org ↵
- Wang, J., Li, M. M., Zhou, L. P., Xie, R. H., Pakhale, S., Krewski, D., & Wen, S. W. (2022). Treatment for grade 4 peripheral intravenous infiltration with type 3 skin tears: A case report and literature review. International Wound Journal, 19(1), 222–229. https://doi.org/10.1111/iwj.13624 ↵
- Gorski, L. A., Hadaway, L., Hagle, M. E., Broadhurst, D., Clare, S., Kleidon, T., Meyer, B. M., Nickel, B., Rowley, S., Sharp, E., & Alexander, M. A. (2021). Infusion therapy standards of practice. Journal of Infusion Nursing, 44(Suppl 1S), S1–S224. https://doi: 10.1097/NAN.0000000000000396.org ↵
- Gorski, L. A., Hadaway, L., Hagle, M. E., Broadhurst, D., Clare, S., Kleidon, T., Meyer, B. M., Nickel, B., Rowley, S., Sharp, E., & Alexander, M. A. (2021). Infusion therapy standards of practice. Journal of Infusion Nursing, 44(Suppl 1S), S1–S224. https://doi: 10.1097/NAN.0000000000000396.org ↵
- This work is a derivative of Clinical Procedures for Safer Patient Care by British Columbia Institute of Technology and is licensed under CC BY 4.0 ↵
As discussed previously, the American Nurses Association (ANA) defines advocacy at the individual level as educating health care consumers so they can consider actions, interventions, or choices related to their own personal beliefs, attitudes, and knowledge to achieve the desired outcome. In this way, the health care consumer learns self-management and decision-making.[1] Advocacy at the interpersonal level is defined as empowering health care consumers by providing emotional support, assistance in obtaining resources, and necessary help through interactions with families and significant others in their social support network.[2]
What does advocacy look like in a nurse’s daily practice? The following are some examples provided by an oncology nurse[3]:
- Ensure Safety. Ensure the client is safe when being treated in a health care facility and when they are discharged by communicating with case managers or social workers about the client’s need for home health or assistance after discharge so it is arranged before they go home.
- Give Clients a Voice. Give clients a voice when they are vulnerable by staying in the room with them while the doctor explains their diagnosis and treatment options to help them ask questions, get answers, and translate information from medical jargon.
- Educate. Educate clients on how to manage their current or chronic conditions to improve the quality of their everyday life. For example, clients undergoing chemotherapy can benefit from the nurse teaching them how to take their anti-nausea medication in a way that will be most effective for them and will allow them to feel better between treatments.
- Protect Patient Rights. Know clients’ wishes for their care. Advocacy may include therapeutically communicating a client’s wishes to an upset family member who disagrees with their choices. In this manner, the client’s rights are protected and a healing environment is established.
- Double-Check for Errors. Know that everyone makes mistakes. Nurses often identify, stop, and fix errors made by interprofessional team members. They flag conflicting orders from multiple providers and notice oversights. Nurses should read provider orders and carefully compare new orders to previous documentation. If an order is unclear or raises concerns, a nurse should discuss their concerns with another nurse, a charge nurse, a pharmacist, or the provider before implementing it to ensure patient safety.
- Connect Clients to Resources. Help clients find resources inside and outside the hospital to support their well-being. Know resources in your agency, such as case managers or social workers who can assist with financial concerns, advance directives, health insurance, or transportation concerns. Request assistance from agency chaplains to support spiritual concerns. Promote community resources, such as patient or caregiver support networks, Meals on Wheels, or other resources to meet their needs.
Nurses must recognize their unique position in client advocacy to empower individuals to provide them with the support and resources to make their best judgment. The intimate and continuous nature of the nurse-patient relationship places nurses in a prime position to identify and address the needs and concerns of their patients. This relationship is built on trust, empathy, and consistent interaction, which allows nurses to gain a deep understanding of their patients' values, preferences, and personal circumstances. By leveraging this close proximity and strong rapport, nurses can effectively advocate for their patients, ensuring that their voices are heard, and their wishes are respected in all aspects of care.[4]
The power of the nurse-patient relationship extends beyond the immediate clinical environment. Nurses often act as liaisons between patients and the broader health care team, facilitating communication and ensuring that patient preferences are integrated into care plans. This advocacy role is crucial in navigating complex health care systems where patients may feel overwhelmed or marginalized. Nurses can help demystify medical jargon, explain treatment options, and support patients in making informed decisions that align with their values and goals. Through education and emotional support, nurses empower patients to take an active role in their own care, enhancing patient autonomy and satisfaction.[5]
In addition to direct patient care, nurses play a pivotal role in identifying systemic issues that affect patient outcomes. Their frontline perspective provides valuable insights into the barriers patients face in accessing quality care, such as socioeconomic challenges, cultural barriers, and institutional policies. By advocating for policy changes and improvements in health care delivery, nurses contribute to creating a more equitable and patient-centered health care system. Their advocacy efforts can lead to the implementation of practices and policies that better address the needs of diverse patient populations, ultimately improving health outcomes on a broader scale.[6]
Nurses' advocacy is also essential in situations where patients are unable to speak for themselves, such as in cases of severe illness, disability, or end-of-life care. In these instances, nurses must be vigilant in recognizing and addressing the needs of vulnerable patients, ensuring that their rights and dignity are upheld. This may involve working closely with families and caregivers, coordinating with interdisciplinary teams, and navigating ethical dilemmas to provide the best possible care for the patient.
As discussed previously, the American Nurses Association (ANA) defines advocacy at the individual level as educating health care consumers so they can consider actions, interventions, or choices related to their own personal beliefs, attitudes, and knowledge to achieve the desired outcome. In this way, the health care consumer learns self-management and decision-making.[7] Advocacy at the interpersonal level is defined as empowering health care consumers by providing emotional support, assistance in obtaining resources, and necessary help through interactions with families and significant others in their social support network.[8]
What does advocacy look like in a nurse’s daily practice? The following are some examples provided by an oncology nurse[9]:
- Ensure Safety. Ensure the client is safe when being treated in a health care facility and when they are discharged by communicating with case managers or social workers about the client’s need for home health or assistance after discharge so it is arranged before they go home.
- Give Clients a Voice. Give clients a voice when they are vulnerable by staying in the room with them while the doctor explains their diagnosis and treatment options to help them ask questions, get answers, and translate information from medical jargon.
- Educate. Educate clients on how to manage their current or chronic conditions to improve the quality of their everyday life. For example, clients undergoing chemotherapy can benefit from the nurse teaching them how to take their anti-nausea medication in a way that will be most effective for them and will allow them to feel better between treatments.
- Protect Patient Rights. Know clients’ wishes for their care. Advocacy may include therapeutically communicating a client’s wishes to an upset family member who disagrees with their choices. In this manner, the client’s rights are protected and a healing environment is established.
- Double-Check for Errors. Know that everyone makes mistakes. Nurses often identify, stop, and fix errors made by interprofessional team members. They flag conflicting orders from multiple providers and notice oversights. Nurses should read provider orders and carefully compare new orders to previous documentation. If an order is unclear or raises concerns, a nurse should discuss their concerns with another nurse, a charge nurse, a pharmacist, or the provider before implementing it to ensure patient safety.
- Connect Clients to Resources. Help clients find resources inside and outside the hospital to support their well-being. Know resources in your agency, such as case managers or social workers who can assist with financial concerns, advance directives, health insurance, or transportation concerns. Request assistance from agency chaplains to support spiritual concerns. Promote community resources, such as patient or caregiver support networks, Meals on Wheels, or other resources to meet their needs.
Nurses must recognize their unique position in client advocacy to empower individuals to provide them with the support and resources to make their best judgment. The intimate and continuous nature of the nurse-patient relationship places nurses in a prime position to identify and address the needs and concerns of their patients. This relationship is built on trust, empathy, and consistent interaction, which allows nurses to gain a deep understanding of their patients' values, preferences, and personal circumstances. By leveraging this close proximity and strong rapport, nurses can effectively advocate for their patients, ensuring that their voices are heard, and their wishes are respected in all aspects of care.[10]
The power of the nurse-patient relationship extends beyond the immediate clinical environment. Nurses often act as liaisons between patients and the broader health care team, facilitating communication and ensuring that patient preferences are integrated into care plans. This advocacy role is crucial in navigating complex health care systems where patients may feel overwhelmed or marginalized. Nurses can help demystify medical jargon, explain treatment options, and support patients in making informed decisions that align with their values and goals. Through education and emotional support, nurses empower patients to take an active role in their own care, enhancing patient autonomy and satisfaction.[11]
In addition to direct patient care, nurses play a pivotal role in identifying systemic issues that affect patient outcomes. Their frontline perspective provides valuable insights into the barriers patients face in accessing quality care, such as socioeconomic challenges, cultural barriers, and institutional policies. By advocating for policy changes and improvements in health care delivery, nurses contribute to creating a more equitable and patient-centered health care system. Their advocacy efforts can lead to the implementation of practices and policies that better address the needs of diverse patient populations, ultimately improving health outcomes on a broader scale.[12]
Nurses' advocacy is also essential in situations where patients are unable to speak for themselves, such as in cases of severe illness, disability, or end-of-life care. In these instances, nurses must be vigilant in recognizing and addressing the needs of vulnerable patients, ensuring that their rights and dignity are upheld. This may involve working closely with families and caregivers, coordinating with interdisciplinary teams, and navigating ethical dilemmas to provide the best possible care for the patient.
Nurses advocate for issues in their communities and their organizations.
Addressing Social Determinants of Health
Advocacy is commonly perceived as acting on behalf of a client, but it can be a much broader action than affecting a single client and their family members. Nurses advocate for building healthier communities by addressing social determinants of health (SDOH). SDOH are the conditions in the environments where people live, learn, work, and play that affect a wide range of outcomes. SDOH include health care access and quality, neighborhood and environment, social and community context, economic stability, and education access and quality. Social determinants of health (SDOH) have a major impact on people’s health, well-being, and quality of life. See Figure 10.2[13] for an illustration of SDOH.[14]

Specific examples of addressing SDOH include the following goals:
- Improving safe housing and public transportation
- Decreasing discrimination and violence
- Expanding quality education and job opportunities
- Increasing access to nutritious foods and physical activity opportunities
- Promoting clean air and clean water
- Enhancing language and literacy skills[15]
SDOH contribute to health disparities and inequities among different socioeconomic groups. For example, individuals who don't have access to grocery stores with healthy foods are less likely to have good nutrition, increasing their risk for health conditions like heart disease, diabetes, and obesity, and potentially lowering their life expectancy relative to people who do have access to healthy foods.[16]
One of Healthy People 2030’s goals specifically relates to advocacy regarding SDOH. The goal states, “Create social, physical, and economic environments that promote attaining the full potential for health and well-being for all.” Across the United States, people and organizations at the local, state, territorial, tribal, and national levels are working hard to improve health and reduce health disparities by addressing SDOH.[17] Read more information about these advocacy efforts in the following box.
Read more about efforts addressing SDOH at Healthy People 2030.


